Pediatric keratoconus can progress faster than many parents expect. In children and teens, the cornea may weaken and change shape quickly, leading to blurred vision, rising glasses power, and trouble with school, sports, and daily life. That is why early diagnosis matters so much.
Early CXL intervention can help slow or stop this progression before the condition causes more serious visual damage. In this blog, you’ll learn what pediatric keratoconus is, why it tends to be more aggressive in younger patients, how corneal cross-linking works, and when to seek expert help. If you are looking into keratoconus treatment for children, understanding the value of timely care is the first step.
What is Pediatric Keratoconus?
Pediatric keratoconus is a condition in which the cornea, the clear front surface of the eye, becomes thin and bulges outward into a cone-like shape. This irregular shape prevents light from focusing properly on the retina, which leads to distorted and blurred vision.
In children, keratoconus is often more concerning because it may worsen at a faster rate than it does in adults. A child may not always notice or report vision changes early, so the condition can advance before it is diagnosed.
Common signs of pediatric keratoconus include:
- Frequent changes in glasses prescription
- Blurred or distorted vision
- Increased sensitivity to light
- Eye rubbing
- Ghosting or double images
- Trouble seeing clearly at night
The key point is simple: pediatric keratoconus is not just “bad eyesight.” It is a progressive corneal disease that needs careful monitoring and, in many cases, early treatment.
Why Early Detection Matters in Children
Early detection gives doctors a better chance to protect vision before the cornea becomes more unstable. This is especially important in young patients because pediatric keratoconus often progresses aggressively during the growing years.
If keratoconus is picked up late, a child may already have:
- Significant corneal thinning
- More irregular astigmatism
- Poorer quality of vision
- Greater dependence on specialty contact lenses
- A higher risk of needing more advanced intervention later
By contrast, early CXL intervention aims to treat the disease while the cornea is still in a more manageable stage. This can help preserve vision and reduce the risk of long-term complications.
Parents should be especially alert if their child has a history of:
- Allergies with frequent eye rubbing
- Asthma or eczema
- A family history of keratoconus
- Rapidly changing vision
- Poor vision that does not improve fully with glasses
Here’s the takeaway: the sooner pediatric keratoconus is identified, the more options there are to stabilize the condition and protect the child’s future vision.
Why Pediatric Keratoconus Can Progress Faster
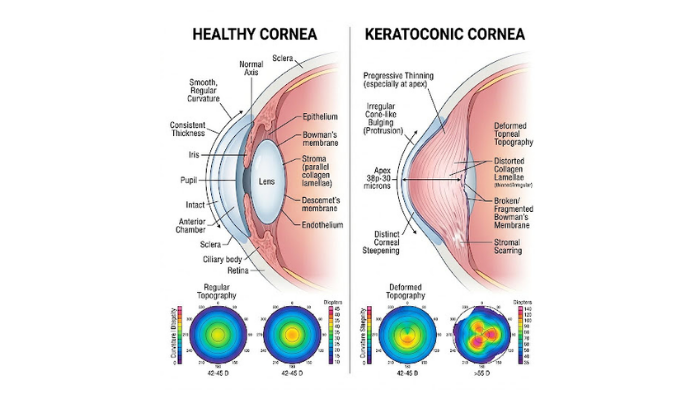
Children are not just small adults when it comes to eye disease. The cornea in younger patients may show faster progression, which means doctors often recommend close follow-up and timely action.
There are a few reasons this matters:
Younger corneas may be more vulnerable
A child’s cornea can change more quickly, and the disease may advance over a shorter period. What seems like a minor prescription shift may actually be a sign of ongoing corneal instability.
Delayed diagnosis is common
Children may struggle to describe what they are seeing. They may squint, move closer to screens, or avoid visual tasks without realizing there is a medical problem.
Progression affects learning and quality of life
Blurred vision can impact reading, classroom performance, confidence, and participation in sports. Early treatment is not only about the eye. It is also about supporting a child’s day-to-day development.
This is why regular eye exams and corneal imaging are so important in at-risk children.
What is Corneal Cross-Linking (CXL)?
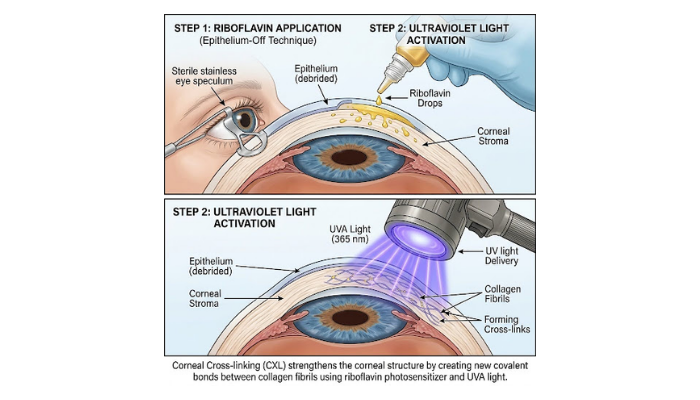
Corneal cross-linking, often called CXL, is a treatment designed to strengthen the cornea and slow or stop the progression of keratoconus. It does this by increasing the natural bonds within corneal tissue.
In simple terms, CXL helps make the cornea more stable.
The procedure generally involves two main steps:
- Riboflavin eye drops are applied to the cornea.
- Controlled ultraviolet-A light is used to activate the riboflavin and strengthen the corneal fibers.
The goal of CXL is not to “cure” keratoconus or restore perfect vision on its own. Its main purpose is to halt progression. Once the disease is stabilized, vision can then be managed more effectively with glasses, contact lenses, or other measures when needed.
That is what makes early CXL intervention such a game changer. It addresses the disease process itself, not just the symptoms.
Why Early CXL Intervention Is a Game Changer
Early CXL intervention can make a major difference in how pediatric keratoconus is managed over time. Instead of waiting for the cornea to worsen, doctors can act earlier to preserve structure and function.
It can slow or stop disease progression
This is the biggest benefit. In children with progressive keratoconus, CXL can reduce the chance that the cornea will continue to steepen and thin.
It helps protect long-term vision
When treatment is done early enough, it may help preserve better visual quality over the long term. Stabilizing the cornea earlier often means there is less distortion to manage later.
It may reduce the need for more complex care
If keratoconus is allowed to advance, patients may need more difficult visual rehabilitation or, in severe cases, corneal transplantation. Early CXL intervention can lower that risk.
It supports better daily functioning
For children and teens, stable vision matters in school, sports, and social life. Treating progression early may help limit future disruption.
The bottom line: early CXL intervention changes the conversation from reacting to damage to preventing it.
When Should a Child Be Evaluated for CXL?
Not every child with irregular vision has keratoconus, and not every child with keratoconus needs immediate treatment. The right timing depends on a detailed clinical evaluation.
A child should be assessed promptly if there is:
- Confirmed pediatric keratoconus on corneal topography or tomography
- Evidence of progression over time
- Increasing corneal steepening
- Thinning of the cornea
- Worsening vision or rising astigmatism
- A strong risk profile with suspicious clinical findings
This is where specialist assessment matters. Decisions about keratoconus treatment for children should be based on careful imaging, symptom review, refraction changes, and the child’s overall eye health.
If there is concern about progression, delaying the conversation may reduce the benefit of timely intervention.
What Parents Should Watch For
Parents often notice the first clues before a diagnosis is made. Knowing what to look for can lead to faster evaluation.
Watch for these warning signs:
- Your child’s glasses prescription changes often
- Vision remains blurry even with updated glasses
- One eye seems much worse than the other
- Your child rubs their eyes often
- They complain of glare, halos, or shadowed vision
- Teachers mention squinting or trouble seeing the board
Common mistake: assuming it is “just changing eyesight”
Many parents think repeated prescription changes are a normal part of growing up. Sometimes they are. But when changes are frequent, uneven, or linked with poor visual quality, pediatric keratoconus should be ruled out.
If you notice these patterns, do not wait for the next routine exam. Schedule a comprehensive eye evaluation.
How Specialist Care Makes a Difference
Managing pediatric keratoconus requires more than a basic vision test. It needs careful diagnosis, advanced corneal imaging, and a treatment plan tailored to a growing child.
An experienced eye specialist can help by:
- Confirming whether keratoconus is present
- Measuring progression accurately
- Deciding if and when early CXL intervention is appropriate
- Guiding post-treatment follow-up
- Coordinating long-term visual rehabilitation if needed
For families seeking expert evaluation and keratoconus treatment for children, choosing a surgeon with experience in corneal disease is an important step.
Why Families Trust Dr. Vinay Agrawal for Pediatric Keratoconus Care
When a child is diagnosed with keratoconus, parents want clarity, experience, and a treatment plan they can trust. Dr. Vinay Agrawal offers expert care focused on accurate diagnosis, timely intervention, and long-term visual protection.
With a patient-centered approach, Dr. Vinay Agrawal works closely with families to explain the condition, review testing findings, and discuss whether early CXL intervention is the right step. That kind of guidance can make a stressful diagnosis feel more manageable.
At Clear Vision Eye Centre, the focus is not only on treating the disease but also on helping children maintain the best possible quality of vision as they grow.
Practical Checklist for Parents
If you are concerned about pediatric keratoconus, here is a simple checklist to follow:
- Schedule a detailed eye exam if your child’s prescription changes often
- Ask whether corneal topography or tomography is needed
- Mention any history of eye rubbing, allergies, or family keratoconus
- Keep records of old prescriptions to track changes
- Do not ignore blurred vision that persists despite new glasses
- Seek specialist advice early if keratoconus is suspected
This checklist can help you move from concern to action without delay.
Conclusion: Early Action Can Protect Your Child’s Vision
Pediatric keratoconus can progress quickly, but early diagnosis and early CXL intervention can make a real difference. By stabilizing the cornea before the disease causes more damage, corneal cross-linking offers an important opportunity to protect long-term vision and reduce future complications.
If your child has frequent prescription changes, blurred vision, or signs that suggest pediatric keratoconus, do not wait. Early evaluation is one of the most important steps you can take. For expert assessment and personalized keratoconus treatment for children, consult Dr. Vinay Agrawal at Clear Vision Eye Centre. Timely care today can help safeguard your child’s sight for the years ahead.
FAQs: Pediatric Keratoconus and Early CXL Intervention
Q: What is pediatric keratoconus?
A: Pediatric keratoconus is an eye condition where the cornea becomes thin and starts to bulge outward into a cone shape. This changes how light enters the eye and can cause blurred vision, glare, ghosting, and frequent prescription changes in children and teens.
Q: How is keratoconus diagnosed in children?
A: Keratoconus is diagnosed through a detailed eye exam and corneal imaging tests such as corneal topography or tomography. These tests map the shape of the cornea and help detect early changes that may not show up on a regular vision test alone.
Q: What are the common signs of keratoconus in children?
A: Common signs include blurry or distorted vision, frequent changes in glasses power, eye rubbing, light sensitivity, and trouble seeing clearly at night. If your child still struggles to see well even after getting new glasses, it is worth getting a closer evaluation.
Q: Why does pediatric keratoconus need early attention?
A: Pediatric keratoconus can progress faster in children than in adults, which means vision may worsen more quickly. Early detection gives doctors a better chance to stabilize the cornea before the condition becomes more advanced.
Q: What is corneal cross-linking (CXL)?
A: Corneal cross-linking, or CXL, is a treatment that strengthens the cornea to slow or stop keratoconus progression. It uses riboflavin eye drops and controlled UV light to make the corneal tissue more stable.
Q: What are the benefits of early CXL intervention?
A: Early CXL intervention can help stop keratoconus from getting worse before major corneal damage occurs. This may help protect long-term vision, reduce future complications, and lower the chance of needing more advanced treatment later.
Q: Is CXL safe for children?
A: CXL is widely considered a safe and effective treatment when performed in properly selected patients by an experienced specialist. As with any procedure, the doctor will evaluate your child’s eye health, corneal thickness, and disease progression before recommending treatment.
Q: Does CXL improve vision right away?
A: The main goal of CXL is to stop keratoconus from worsening, not to provide instant vision correction. Some children may notice visual improvement over time, but many still need glasses or contact lenses after treatment.
Q: When should I consult a specialist for my child?
A: You should consult a specialist if your child has frequent prescription changes, blurred vision that does not improve well with glasses, or signs of keratoconus on an eye exam. Early specialist care is especially important if symptoms are getting worse or there is a family history of keratoconus.
Q: Are some children more at risk for keratoconus?
A: Yes. Children with a family history of keratoconus, frequent eye rubbing, allergies, asthma, or eczema may have a higher risk. If your child falls into one of these groups, regular eye exams and early screening can be very helpful.
Q: Can keratoconus be treated without surgery?
A: In early or mild cases, vision may be managed with glasses or specialty contact lenses, but these do not stop the disease from progressing. If the cornea is changing over time, CXL may be recommended to help preserve eye shape and vision.
Q: How do I know if my child may need CXL?
A: A child may need CXL if tests show progressive keratoconus, increasing corneal steepening, or thinning of the cornea. The best way to know is through a specialist evaluation with proper imaging and follow-up.
Q: What should parents do if they suspect pediatric keratoconus?
A: Schedule a comprehensive eye evaluation as soon as possible. If keratoconus is suspected, early testing and specialist review can make a big difference in protecting your child’s long-term vision.

