When the clarity of your world begins to blur due to the thinning and bulging of the cornea, the diagnosis often points toward Keratoconus. This progressive eye condition can be daunting, but medical advancements have introduced life-changing interventions like Corneal Collagen Cross-Linking (CXL). At our facility, we prioritize a patient-centric approach to vision restoration, ensuring that every individual receives a bespoke path to recovery. Understanding the science behind the condition is the first step toward reclaiming your sight.
The cornea, which acts as the eye’s outermost lens, requires a specific structural integrity to focus light correctly. When this structure weakens, it assumes a cone-like shape, leading to significant visual distortion that glasses often cannot fully correct. Navigating the complexities of ocular health requires a blend of advanced technology and deep clinical empathy. We believe that informed patients make the best decisions for their long-term well-being, which is why we emphasize education alongside our clinical excellence. By focusing on stabilizing the corneal tissue early, we can prevent the need for more invasive procedures later in life.
Our commitment to excellence ensures that you are supported through every stage of the diagnostic and treatment process. If you are seeking specialized care, finding a premier destination for Keratoconus treatment in Mumbai is essential for stabilizing your vision and preventing further deterioration.
Understanding the Mechanics of Keratoconus
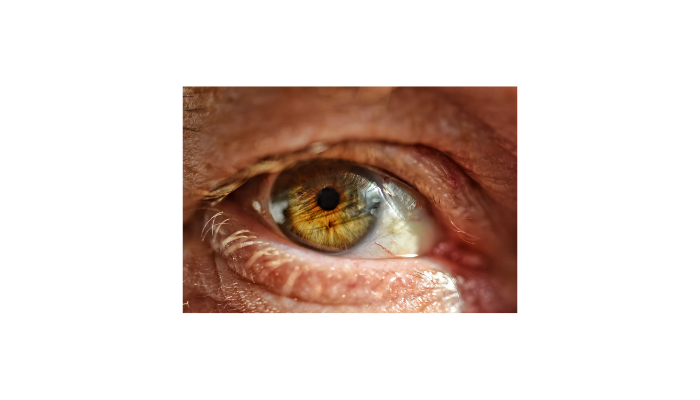
Keratoconus typically manifests during the teenage years or early twenties. It begins subtly, often mistaken for simple nearsightedness or astigmatism. However, as the corneal fibers weaken, the eye’s surface becomes irregular. This irregularity scatters light rather than focusing it sharply on the retina. Symptoms such as increased sensitivity to glare, frequent changes in eyeglass prescriptions, and “ghosting” around images are common red flags.
The primary objective of modern intervention is not just to improve sight but to halt the progression of the “bulge.” This is where CXL becomes the gold standard. By combining Riboflavin (Vitamin B2) drops with Ultraviolet-A light, surgeons can form new bonds between corneal collagen fibers. Think of it as adding structural “anchors” to a weakening wall; it reinforces the cornea, making it stiffer and more resistant to further thinning.
Expert Guidance in Corneal Care

Dr. Vinay Agrawal, a leading figure in ocular health, emphasizes that early detection is the most powerful tool in managing this condition. With over three decades of dedicated ophthalmic practice, he has cultivated a reputation for precision and care. Having completed his M.B.B.S. and M.S. in Ophthalmology, followed by a D.N.B. and a prestigious fellowship at the L.V. Prasad Eye Institute, his expertise is multifaceted. He is widely recognized as a Keratoconus Specialist in Mumbai, bringing a wealth of knowledge in cataract, cornea, and refractive surgeries. His long-standing commitment to the field has helped countless patients navigate the complexities of corneal diseases with confidence and clarity.
The Science Behind Collagen Cross-Linking (CXL)
The CXL procedure itself is minimally invasive and performed as an outpatient task. There are two primary methods: “Epi-off” and “Epi-on.” In the traditional Epi-off method, the thin outer layer of the cornea (the epithelium) is gently removed to allow the Riboflavin drops to penetrate the deeper corneal tissue more effectively.
In the Epi-on method, the epithelium is left intact. While the latter offers a quicker recovery time, the Epi-off method is often preferred for its long-term efficacy in strengthening the corneal bonds. Once the drops have saturated the cornea, the UV-A light is applied for a specific duration. This photochemical reaction is the “cross-linking” that gives the procedure its name.
Recovery and Post-Operative Expectations
Post-operative care is just as critical as the surgery itself. Patients may experience some discomfort or a “gritty” sensation in the days following the procedure, which is a normal part of the epithelial healing process. Medicated eye drops are prescribed to manage inflammation and prevent infection. During this recovery phase, it is vital to avoid rubbing the eyes, as the tissue is still settling into its newly reinforced state. Most patients can return to their daily routines within a week, though visual stabilization may take a few months.
It is important to note that CXL is primarily a stabilizing procedure. At the same time, it can slightly improve corneal shape; however, many patients will still require contact lenses or glasses to achieve their best possible vision.
Why Specialized Surgical Expertise Matters
The impact of this treatment extends beyond the clinical results. For a young person struggling with declining vision, stabilizing the cornea means preserving their independence and career prospects. It significantly reduces the likelihood of needing a corneal transplant, which is a much more complex and invasive surgery. When considering such an important procedure, it is vital to consult a seasoned Keratoconus Surgeon in Mumbai who can provide a comprehensive evaluation using advanced topography and tomography mapping. These diagnostic tools allow the specialist to create a digital “map” of the eye, identifying the exact areas of thinning and irregularity.
Advanced Technology at Your Service
Choosing the right facility is a decision that impacts your quality of life for years to come. Clear Vision Eye Centre stands at the forefront of ophthalmic innovation, offering a sanctuary for those facing vision challenges. The center is equipped with the latest diagnostic and surgical technology, ensuring that every patient benefits from international standards of care.
Whether it is a routine check-up or a specialized Keratoconus Surgery in Mumbai, the focus remains on delivering outcomes that enhance the patient’s daily experience of the world. The synergy between technology and human touch defines the clinic’s philosophy.
A Hub for International Medical Standards
For those residing outside the city, the local experts’ reputation makes this a preferred hub for Keratoconus treatment in India.
The blend of cost-effectiveness and high-tier medical skill attracts patients from across the globe. Beyond surgery, the long-term management of Keratoconus involves specialized lens fitting, such as scleral or Rose-K lenses, which provide superior comfort and visual acuity compared to standard contact lenses. A holistic approach ensures that the patient is not just “treated” but is “managed” throughout their lifetime.
Protecting Your Sight for the Future
Vision is perhaps our most precious sense, and protecting it requires proactive measures. If you have been told your astigmatism is worsening rapidly or if your vision feels “distorted” despite new glasses, it is time to seek a specialist’s opinion.
The evolution of CXL has transformed Keratoconus from a sight-threatening mystery into a manageable condition. By reinforcing the eye’s natural architecture, we provide a foundation for a clearer, brighter future. Trusting your eyes to experts who have spent decades perfecting these techniques ensures that you are in the safest possible hands.
With the right intervention at the right time, the progression of Keratoconus can be halted, allowing you to live your life without the constant fear of losing your sight. For anyone navigating this journey, securing the best Keratoconus treatment in Mumbai is the definitive step toward lasting ocular stability.
Take the First Step Towards Clearer Vision
Don’t let progressive vision loss hold you back from the life you deserve. Early intervention is the key to successfully managing Keratoconus and avoiding the need for more invasive transplants.
At Clear Vision Eye Centre, we combine world-class technology with the compassionate expertise of Dr. Vinay Agrawal to deliver the highest standard of corneal care. Whether you are seeking a second opinion or are ready to schedule your cross-linking procedure, our team is here to guide you every step of the way.
Schedule your comprehensive corneal evaluation today and protect your sight for tomorrow.
Frequently Asked Questions (FAQs)
1. Is Corneal Collagen Cross-Linking (CXL) painful?
The procedure itself is painless as numbing drops are used. However, you may experience some discomfort, redness, and a sandy sensation in the eye for 3 to 5 days following the procedure as the epithelium heals.
2. Can CXL cure Keratoconus?
CXL is not a cure in the sense that it reverses the condition entirely. However, it is highly effective at halting the progression of the disease. It strengthens the cornea to prevent further bulging.
3. Will I still need glasses or contact lenses after the treatment?
Yes, most patients still require vision correction. CXL stabilizes the eye, making it easier to fit contact lenses (such as scleral or RGP lenses) and helping ensure your prescription doesn’t change rapidly.
4. How long does the CXL procedure take?
The entire process usually takes about 30 to 60 minutes per eye, depending on the technique your surgeon uses (Epi-on or Epi-off).
5. At what age should one get CXL?
CXL is most effective when performed as soon as progression is detected, which is often in the teenage years or early adulthood. However, it can be performed at any age if the cornea is still thick enough and progression is documented.

